Laurie's Blogs.
Apr 2026
Canine Hypermobility Syndrome and Ehlers-Danlos Syndrome: A Practical Guide for Rehab
In rehab clinics, we’re used to seeing dogs with loose joints, recurrent sprains, or that “too bendy” feel during assessments. But what happens when it’s not just one joint or a simple orthopedic issue? Enter canine hypermobility syndrome and its close (sometimes overlapping) cousin, Ehlers-Danlos syndrome (EDS), also known as cutaneous asthenia. These connective-tissue disorders are rare but can dramatically affect how we approach stability, exercise prescription, and long-term management.
While human EDS gets a lot of press for its multi-system effects, the canine versions are often subtler in joints but can still pack a punch—especially when skin fragility or behavioral quirks show up alongside the laxity. Let’s break it down in a way that helps us spot it early, manage it conservatively, and keep these pups moving comfortably. Recent insights from human hypermobility literature add even more practical depth to our rehab toolbox, since the core principles of building dynamic stability translate beautifully to our four-legged patients.
What Exactly Are We Talking About?
Canine hypermobility syndrome refers to generalized joint laxity driven by connective-tissue changes, often without the full-blown skin involvement of classic EDS. EDS (cutaneous asthenia) is a group of inherited disorders caused by defects in collagen synthesis or structure—most commonly mutations in genes like COL5A1 that affect type V collagen. This leads to skin that stretches like taffy and tears with minimal trauma, plus variable joint hypermobility.
In dogs, skin signs usually dominate (hyperextensibility, easy bruising, poor wound healing, “cigarette-paper” scars), but joint laxity can coexist—think patellar luxations, carpal hyperextension, or even atlantoaxial instability in severe cases. Unlike humans, it’s uncommon to see both dramatic skin and joint changes in the same dog, but when they overlap, the connective-tissue weakness is systemic. Breeds over-represented include English Springer Spaniels, but it pops up in Labs, mixed breeds, Shih Tzus, and others. Inheritance is usually autosomal dominant, with de novo mutations reported.
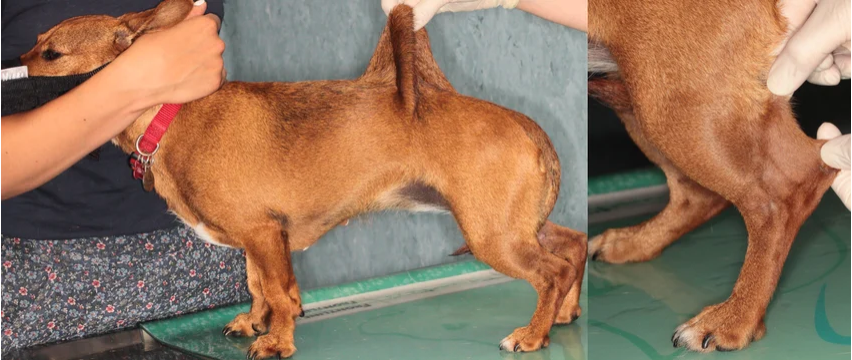
From: https://www.researchgate.net/publication/334813816_Compound_heterozygosity_for_TNXB_genetic_variants_in_a_mixed-breed_dog_with_Ehlers-Danlos_syndrome
A fascinating parallel to human medicine: one large study of over 5,500 assistance dogs found a clear link between hip hypermobility (measured by PennHIP distraction index) and higher “excitability” scores—think difficulty calming down, emotional arousal, and even some aggression toward familiar dogs. Females and certain breeds (Goldens especially) scored higher. This suggests we should screen behavior alongside biomechanics.
Spotting It in the Clinic
Classic red flags:
• Skin that stretches >15–20% (extensibility index often >20–26% in confirmed cases) and recoils slowly.
• Frequent skin tears, seromas, or delayed healing despite good suturing.
• Joints that feel “mushy” or demonstrate excessive range (e.g., >180° carpal/tarsal extension, easy patellar luxation).
• History of recurrent minor injuries or “loose” gait without obvious trauma.
• Occasionally: ocular issues (entropion, keratoconjunctivitis sicca, lid laxity) or vascular fragility.
Diagnosis is clinical first (skin stretch test + whole-dog orthopedic/neuro exam), then supported by skin biopsy (collagen dysplasia, “cauliflower” fibrils on electron microscopy), and increasingly by genetic testing for known variants. Rule out mimics like other connective-tissue issues or nutritional deficiencies.
Clinical Utilization: How I’d Approach These Cases as in a Rehab Context
From a physiotherapy standpoint, the goal is the same as in human hypermobility/EDS: build dynamic stability through neuromuscular control rather than relying on passive structures. The human literature on JHS/HSD (often managed in rehab settings) reinforces this perfectly and gives us evidence-based tactics we can adapt directly for dogs—where canine-specific rehab data is still emerging but the principles hold strong.
Here’s how I would translate the science into the canine rehab clinic:
1. Whole-dog assessment first. Always start with spinal and pelvic-girdle mobility—sacroiliac dysfunction is surprisingly common and can amplify limb instability. Correct that before loading the periphery. Use motion palpation and instability tests (adapted equivalents to human prone instability or apprehension signs) to flag segments that need gentle, targeted mobilizations only—never high-velocity thrusts on lax areas.
2. Proprioception and neuromuscular re-education as the absolute foundation. These dogs (like their human counterparts) often have impaired joint-position sense, leading to clumsiness and recurrent micro-trauma. Prioritize balance pads, wobble cushions, cavaletti, three-leg stands, and weight-shifting drills. In human protocols, activities like Pilates or Tai Chi equivalents shine here; for dogs, think slow, controlled weight shifts or “bird-dog” style four-point kneeling progressions on foam. Avoid end-range stretching—focus on controlled mid-range activation.
3. Strengthen within controlled range—no end-range locking or overstretching. Light resistance training (TheraBand walks, sit-to-stand on foam or vibration platforms, closed-chain exercises) can positively influence collagen remodeling, just as seen in human studies. Adapt core-stability moves like pelvic tilts in sternal recumbency (gentle anterior/posterior rocking of the pelvis while the dog lies in a sphinx or sternal position on a mat, using a treat lure to encourage small, controlled movements without shifting the feet).

4. Hydrotherapy, vibration platforms, and supportive tools are gold. Underwater treadmill gives buoyancy and resistance without joint pounding. Whole-body vibration (with sit-to-stand or three-leg holds) boosts proprioception and muscle firing with minimal skin shear. Consider kinesiology taping, soft splints, or compression garments for proprioceptive feedback and temporary support—mirroring human use of braces or kinesiology tape to enhance joint awareness and reduce instability episodes.

5. Behavioral and lifestyle considerations. High excitability? Short, focused sessions with calm-down cues. Teach owners to avoid high-impact play, tight harnesses that cause shear, and prolonged static postures. Optimize home ergonomics—padded environments, neutral spine cues during activity.
6. Manual therapy with caution. Gentle mobilizations or soft-tissue work on hypomobile segments only; expect slower progress and possible post-treatment soreness. The human data shows stabilization programs reduce pain and improve function, but recovery takes time due to proprioceptive retraining—set realistic expectations with clients.
7. Monitor, progress slowly, and educate. Reassess frequently—hypermobility doesn’t “fix,” but improved motor control can dramatically cut injury frequency. Many of these dogs live very functional lives with dedicated home programs. Skin protection and owner buy-in are non-negotiable.
Bottom line: these cases are incredibly rewarding. Instead of chasing one joint, we get to play detective across the whole kinetic chain and design creative, progressive programs that truly change quality of life. The human hypermobility rehab framework gives us a ready-made roadmap that fits seamlessly with what we already do in canine physio.
If you’re seeing more “bendy” dogs in your caseload lately, you’re not imagining it—awareness is growing. Screen for hypermobility early, think systemically, and lean on conservative rehab. Your patients (and their owners) will thank you.
References
• Bowen J, Fatjó J, Serpell JA, Bulbena-Cabré A, Leighton E, Bulbena A. (2019). First evidence for an association between joint hypermobility and excitability in a non-human species, the domestic dog. Scientific Reports. PMC6565730.
• Bauer A, Bateman JF, Lamandé SR, et al. (2019). Identification of Two Independent COL5A1 Variants in Dogs with Ehlers–Danlos Syndrome. Genes, 10(10):731. https://www.mdpi.com/2073-4425/10/10/731.
• Kraeling M. (2020). Treatment of Systemic Hypermobility in Dogs. Canine Fitness blog. https://www.caninefitness.com/index.php?pid=35&name=Blog&bid=112&title=Treatment-of-Systemic-Hypermobility-in-Dogs
• Rasch SN. (2017). Surgical and medical treatment of ocular disease in a dog with Ehlers–Danlos syndrome. Clinical Case Reports. PMC5458014.
• ChiroUp. (n.d.). Joint Hypermobility Syndrome and Hypermobility Spectrum Disorder: Chiropractic Diagnosis and Treatment. https://chiroup.com/blog/joint-hypermobility-syndrome-and-hypermobility-spectrum-disorder-chiropractic-diagnosis-and-treatment (Human hypermobility management principles adapted for canine translational application).


